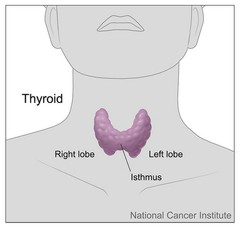
I get a lot of questions about the thyroid and it’s role in weight loss so I wanted to spend some time explaining the basics of hypothryoidism and the role of the thryoid.
What is hypothryoidism?
Hypothyroidism is a medical term that means that your thyroid is underactive and therefore not producing enough thyroid hormone. The vast majority of people with thyroid disease have a form of hypothyroidism called Hashimoto’s Thyroiditis, an autoimmune condition that inflames the thyroid and causes hypothyroidism.
Am I affected?
Are you tired, cold, depressed or constipated? Do you notice that your eyebrows are thinning? Is your hair thinner and is your skin drier? Do you struggle to lose weight even though your diet is relatively well-balanced? Do your lab reports indicate high cholesterol, vitamin or mineral deficiency or blood sugar issues? While these signs and symptoms might be due to a number of issues, you might have an undiagnosed thyroid condition called hypothyroidism or underactive thryoid. You also might have something called sub-clinical hypothyroidism which means that your thryoid labs might only be mildly abnormal but you might be experiencing symptoms anyway. Most medical providers in this case like to take “watch and wait” strategy until you feel really awful or your labs are a total mess I suppose. My philosophy. is that if you aren’t feeling well, we should act.
Hypothroidism is often undiagnosed.
Many clinicians only order a test called Thyroid Stimulating Hormone (TSH). Ordering this test alone does not tell the whole picture. In fact, it is possible for TSH to be normal but to still have thyroid imbalance that is negatively affecting your health and well-being.
When lab tests are relatively normal or more complex labs haven’t been ordered, hypothyroidism or sub-clinical hypothyroidism is frequently missed. In my practice, I have uncovered many cases of otherwise undiagnosed thryoid issues because the labs that help clinicians diagnose this condition are often not ordered and because the symptoms of thyroid disease are often just considered a “normal” part of aging.
Thyroid disease is very common
The American Thyroid Association tells us that approximately 20 million Americans have some form of thyroid disease and up to 60 percent of them are unaware of their condition. One in eight women is effected. Women are five to eight more likely than men to have thyroid issues.
What should I do if I suspect that I have thyroid disease?
The first step is to get properly tested.
To fully research whether or not you have thyroid disease I suggest you also get tested for: TSH, Free T3, Free T4, Total T4, TPO (thyroid peroxidase) and anti-thyroglobulin antibodies. These last two markers are an indication of autoimmune thyroid disease. This is important to test for because, Hashimoto’s Thyroiditis, an autoimmune disease that affects the thryoid, is the number one cause of thyroid disease in the US.
I also recommend working with a functional medicine provider who can help you address and treat the root cause of thyroid disease and, importantly, have a mechanism to track your progress and adjust your treatment as needed, rather than just ignoring the till it gets worse or going directly on a medication.
Next week I will continue my discussion of thyroid disease with an overview of hypothryoidism and the thyroid.
Please note that this article is for information purposes only. Always check with your medical provider before starting any treatment.